Colon Cancer
Anatomy and Surgery for Colon Cancer
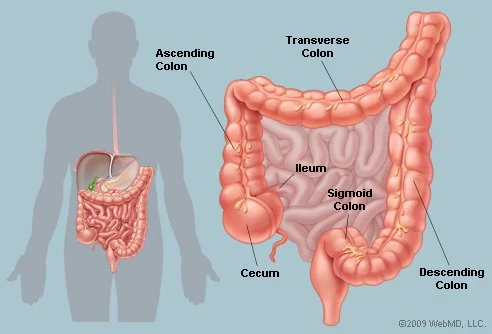
The colon, otherwise known as the large intestine, is the final portion of the digestive tract. It absorbs water, stores and eliminates stool. The colon is comprised of many layers, some of which are the outer muscular layers, which propel stool through the colon and the inner mucosal layers which produce mucus and aid in absorption.The tissue in the colon can change, causing growths, either cancerous or benign (polyps), to form within the colon wall.
About the colon
Your body has approximately 5 feet of large intestine. If only a part of your colon is removed through surgery, enough usually remains to allow you to have a normal lifestyle and digestive function. Sometimes patients find that they initially have an increase in the number of bowel movement immediately after surgery, but they usually return to their normal bowel routine over the following year as their remaining colon adjusts.
Polyps
A polyp is a benign, or non-cancerous, growth that occurs on the colon’s inner lining. They can vary in size. The larger the polyp, the more likely it is that it can become cancerous. Small polyps are often removed by gastroenterologists during colonoscopies. If they are completely removed and are found to be benign after microscopic evaluation, no further management is necessary. Otherwise, having those polyps, which can not be removed by colonoscopy, surgically resected as soon as possible through colon surgery will help prevent them from becoming cancerous.
Colon Cancer
Cancer on the colon wall is a group of abnormal cells that grow at an uncontrolled rate. They can continue to grow and spread to other parts of the body such as lymph nodes (glands), liver and lungs. When it has spread, it said to be metastatic. Cancers should be removed through surgery as soon as they are detected to prevent them from spreading, or metastasizing.
Symptoms and Diagnosis
Many patients are asymptomatic (no symptoms), this is why screening colonoscopies are so important.
Regular screening, beginning at age 50, is the key to preventing colorecectal cancer. Fecal Occult Blood Testing, which checks for hidden blood in three consecutive stool samples should be done every year.
Colonoscopy, where physicians use a flexible, lighted tube/camera (colonoscopy) to look at the interior walls of the rectum and the entire colon, should be done every 10 years. During this procedure, samples of tissue may be collected for closer examination or polyps may be removed.
Higher risk individuals should speak with their primary care physician or gastroenterologist about early or more frequent screening.Here at Suncoast Surgical Associates, we have well-established relationships with all local gastroenterologists and can help direct you if you do not already have a relationship with a gastroenterologist.
Colon Cancer Surgery
To treat colon cancer, surgical removal of the affected portion of the colon is necessary. After the growth and surrounding portion of the colon are removed, the colon is reconnected and normal bowel function is restored. At the same time, we take out regional lymph nodes in order to assess if the cancer has spread so that we can appropriately treat you.
Prior to surgery, we will want to check if the cancer has spread to other parts of the body and may order certain blood tests and scans to assess this. If your cancer has spread, chemotherapy may be needed as an adjunct and we will assist you in streamlining the process by working with your oncologist.At Suncoast Surgical, we are trained in the most advanced techniques to perform all colon surgeries using minimally invasive techniques. This leads to less pain and decreased length of hospital stay. We perform all our colon surgeries with two surgeons and are proud of our outcomes.
Preparing for Colon Surgery
Prior to surgery you should review any prescriptions you take with your doctor, since some may need to be discontinued a week or days before your colon surgery, such as drugs that interfere with blood clotting such as aspirin and Plavix.
You will either have a phone or in-person interview with the hospital anesthesia team to discuss your procedure. They will notify you of medications you should stop or take the day of surgery and let you know what time you should come in for your surgery. You will be asked to come in a few hours earlier than your scheduled surgery time.
A “prep” in order to clean your colon out prior to surgery is often required. We will go over the specific prep required for your surgery at your consultation.
On the day of your surgery :
No eating or drinking after midnight the night before your surgery
Take any drugs your doctor said you may take with a sip of water
Shower the night before or the morning of your surgery
After Colon Surgery
Most patients can expect to stay in the hospital from two to seven days depending on how they progress.
You will soon be started on a clear liquid diet and advanced as appropriate to a soft diet until healing is complete.
You will be seen in our office over the next couple months. You should begin to feel normal again after about six weeks, but should avoid heavy lifting and strenuous exercise as these may increase the possibility of hernia formation. You may still tire easily for several months as your body finishes the healing process. You should be sure to rest whenever you feel fatigued.You may be able to resume normal activities after six weeks, and should expect to take time off from work for four to six weeks.
After you have healed, you should follow a high-fiber, well-hydrated, low-fat diet as you resume your daily lifestyle. Fiber supplementation is often necessary as many diets have inadequate amounts of fiber. The daily recommended fiber intake is 30-40gm of fiber depending on your age, stature and weight. Supplements come in all forms, dissolvable powders, capsules and candies. They are well-tolerated and will promote good intestinal health.